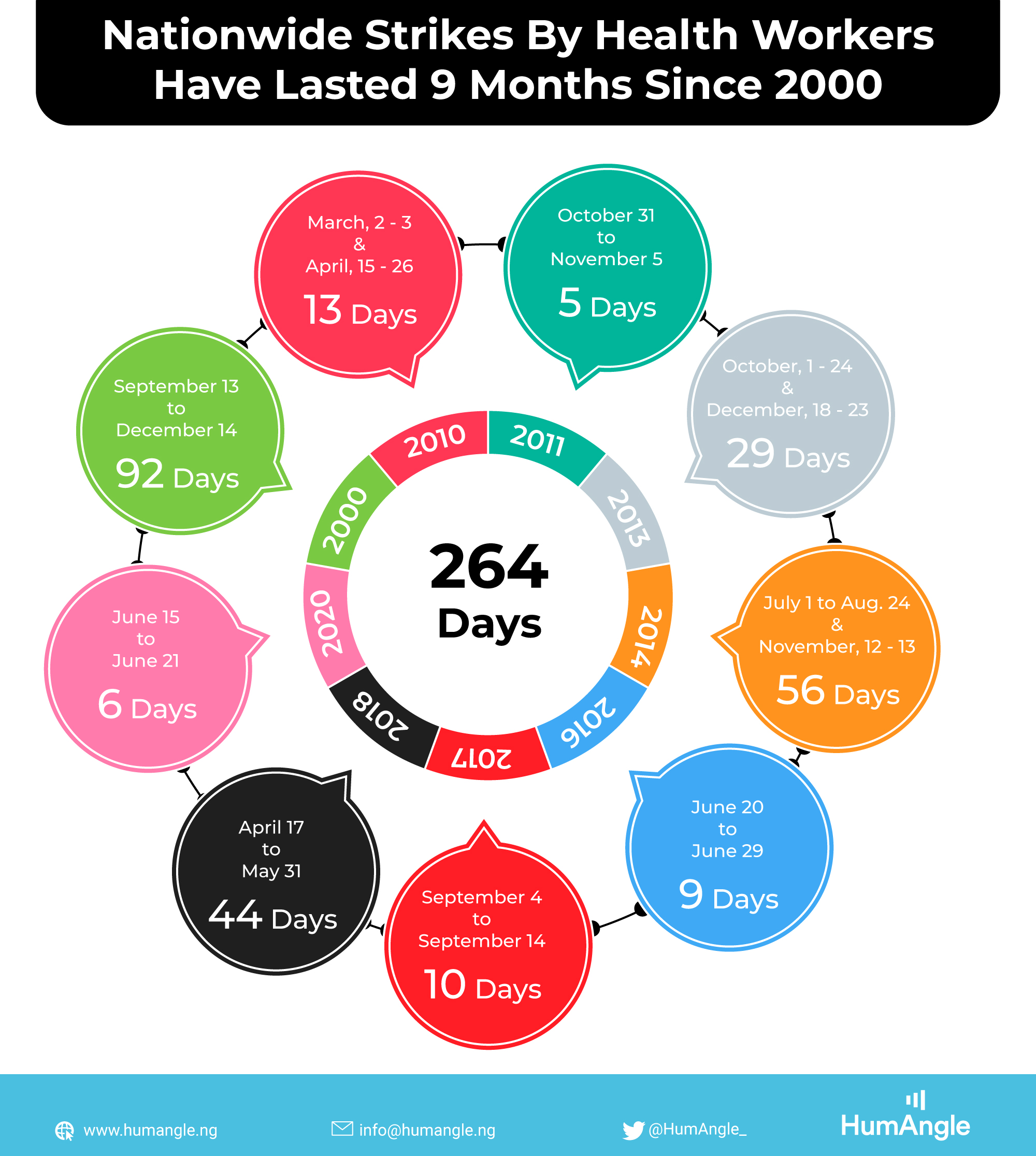
Timeline: Nationwide Strikes By Health Workers Have Lasted 9 Months Since 2000

Hospitals are supposed to be open to the public at all times, but this is not the case in Nigeria where services at state-owned health facilities are often brought to grinding halt by industrial actions.
HumAngle checked reports between 2000 and 2020 and discovered that health workers have gone on nationwide strikes for at least 264 days (roughly nine months).
Since 2010, the country has barely gone two years without a strike by health workers that affected all the states. The aggrieved unions are usually the National Association of Resident Doctors (NARD), Nigeria Medical Association (NMA), Joint Health Sector Unions (JOHESU), Association of Medical Laboratory Scientist of Nigeria (AMLSN) and National Association of Nigerian Nurses and Midwives (NANNM).
The actions documented were 12, during which the unions threatened to stop work and at other times over unresolved issues.
The issues triggering the strikes and outcries have not changed significantly since the start of the new millennium. They range from salary structures to payment of arrears, welfare packages, quality of hospital equipment, funding for training programmes, among others.
The data collected by HumAngle focussed only on nationwide industrial actions but health facilities in many states across the country have also been shut down at various times because of staff grievancesㅡwith such strikes oftentimes lasting longer.
In 2015, a strike by resident doctors crippled the University College Hospital, Ibadan, for 108 days, and another at Ladoke Akintola University of Technology (LAUTECH) Teaching Hospital lasted up to five months.
A review of industrial actions between April 2016 and April 2017 showed that there were at least 17 across the country, out of which six were primary within the healthcare system. Many of the strikes have been recorded to have caused the deaths of patients who could not afford services at private hospitals.
“The entire health system is disrupted as strikes are mostly nationwide except for the few that have been restricted to individual hospitals,” noted Felix Abrahams Obi, a Research Fellow and Research Uptake Officer at University of Nigeria Health Policy Research Group.
“This means that hospitals are closed down and entrances are locked. The wards stay open but the hospitals are forced to run with a skeletal staff. This means there aren’t any doctors to do ward rounds or prescribe drugs to patients and no new patients can be admitted,” he added.
“The impact of these strikes are worse when they coincide with national health emergencies such as Ebola viral disease, Lassa fever or cholera outbreaks or even man-made emergencies like Boko Haram suicide bombings where there are mass casualties.
“In one case in January 2015, people who were injured in a bomb explosion in Adamawa State in northeastern Nigeria were not given adequate medical care due to a strike.”
The Ministry of Labour and Employment’s poor handling of labour disputes has been identified as one of the causes of unending strikes. Out of 6,647 industrial disputes that broke out between 1960 and 1988, at least 60 per cent (3,954) degenerated into strikes.
Participating in a 2018 survey, 16.7 per cent of physicians gave poor staff welfare as the commonest cause of strikes and 13.9 per cent blamed non-payment of salaries. Others pointed at problems with management, poor hospital infrastructure, poor guidelines and services, as well as inter-professional disputes.
Timeline of industrial actions:
September 2000: Members of the National Association of Resident Doctors (NARD) went on strike, as confirmed in a report by Post Express. They demanded the payment of salaries withheld during a previous strike in 1998/1999, “arrears accruing from the 150 per cent increase in call duty with effect from September 1998 till January 1999, and immediate implementation and circularisation of the agreement reached by the inter-ministerial panel that looked into the health sector wage crisis. The strike lasted for three months.
Aside poor welfare packages and working conditions, the doctors also complained about the decline in the quality of health service owing to neglect from the military era. The strike began on September 13, 2000, and ended on December 14, 2000, after government officials promised to meet their demands. The action was reported to have incapacitated many state-run hospitals.
March 2010: After giving a 21-day ultimatum to the Federal Government, NARD embarked on a nationwide two-day warning strike from March 2 to March 3 and later embarked on an indefinite strike that lasted from April 15 to April 26.
The doctors were agitating for a better-funded and restructured training programme and better conditions of service. On August 9, the Federal Government set up the Ministerial Committee on Review of Residency Training in Nigeria to recommend adjustments that would be made to the residency programme.
October 2011: The Association of Medical Laboratory Scientist of Nigeria (AMLSN) started a five-day nationwide work-to-rule industrial action on October 31. The body complained of encroachment on their scheme of service by counterparts in pathology and preserving the professional rights of its members.
October 2013: NARD members went on strike between October 1 and October 24, citing the “nonchalant attitude of the Federal Government to articulate a comprehensive guideline for residency training, withholding of entitlements, and victimisation of doctors.
It signed a memorandum of understanding with the government on October 21, but the following March, the association threatened a fresh strike because the government was yet to implement the provisions of the agreement.
December 2013: NMA went on a five-day nationwide industrial action, which commenced on December 18 and was called off on December 23, after alleging that the federal health ministry was not serious about its demands.
It had issued a 21-day ultimatum in September. It then threatened to go on a full-blown strike on January 6, 2014, if its demands were not met.
The last time the association had gone on a nationwide strike was between 1983 and 1985, at which time Muhammadu Buhari was the military head of state. Doctors across the country downed tools over poor hospital facilities and healthcare delivery, but NMA’s leaders were detained and the association banned until 1986.
July 2014: NMA declared an indefinite nationwide strike “to save the health care delivery system from anarchy that is palpably imminent” and because of the way the government was “taking it for granted”. The association objected to how non-doctors were allowed to function as consultants in hospitals.
The strike, which commenced on July 1, was called off on August 24 after assurances from the Federal Government to address some of the association’s demands.
During the strike, the government announced the sacking of all resident doctors (about 14,000) who constituted the majority in the association. They were later reinstated after the suspension of the strike.
November 2014: The Joint Health Sector Unions (JOHESU) embarked on an industrial action from November 12 to November 13 to demand the payment of arrears by the Federal Government, ratification of salary adjustments, among other things.
June 2016: NARD embarked on a nationwide indefinite strike between June 20 and June 26 over the non-payment of entitlements and the lack of residency training guidelines. It said it suspended the strike to give the government time to implement the agreement reached.
During the strike, the health ministry had directed that doctors who withdrew their services be fired and replaced with new applicants. Around the same time, the National Association of Nigerian Nurses and Midwives (NANNM), also embarked on an indefinite strike. On June 22, JOHESU commenced a seven-day warning strike, making all workers at federal hospitals to down tools.
September 2017: Rejecting the terms of an agreement reached with the Federal Government the previous week, NARD declared a nationwide strike. The action lasted between September 4 and September 14.
The doctors complained about salary shortfalls between 2016 and 2017, delay in promotion, failure to capture members on the Integrated Personnel Payment Information System and failure to remit pension contributions.
April 2018: Health workers under the aegis of JOHESU embarked on a “mega strike”, which lasted for 44 days, between April 17 and May 31. In May, state and local government health workers joined the strike. The industrial action was called off following an order from the National Industrial Court compelling the striking workers to resume.
The strike paralysed activities at both state and federal health institutions and led to the death of many. Members of the union had been demanding an increase in pay and improved working conditions since 2014.
“This is the most unprecedented strike in the history of the health sector because not only federal but both states and local governments joined for the first time,” JOHESU National Vice-Chairman, Ogbonna Chimela, told journalists.
“The other ones (previous strikes) lingered for months but the state and LGAs did not join. This is very unprecedented; though it’s not the best but government made it so,” Chimela added.
Some days after JOHESU called off its strike, NARD threatened a fresh action and accused the government of ignoring its “legitimate agitations”.
June 2020: NARD members in state-run hospitals, with the exemption of COVID-19 treatment centres, stopped working to protest the inadequacy of personal protective equipment for doctors, the size of hazard allowance provided, illegal deductions, and budget funding for residency training.
The strike lasted from June 15 to June 21. Prior to the industrial action, the association had given a two-week ultimatum to the federal and state governments. And as NARD was calling its members to work, JOHESU threatened to call out its members on strike over poor working conditions and unfulfilled promises by the government.
Support Our Journalism
There are millions of ordinary people affected by conflict in Africa whose stories are missing in the mainstream media. HumAngle is determined to tell those challenging and under-reported stories, hoping that the people impacted by these conflicts will find the safety and security they deserve.
To ensure that we continue to provide public service coverage, we have a small favour to ask you. We want you to be part of our journalistic endeavour by contributing a token to us.
Your donation will further promote a robust, free, and independent media.
Donate Here